A
B
C
D
E
F
G
H
I
J
K
L
M
N
O
P
Q
R
S
T
U
V
W
X
Y
Z
Click a letter to see a list of conditions beginning with that letter.
Click 'Topic Index' to return to the index for the current topic.
Click 'Library Index' to return to the listing of all topics.
Understanding Methacholine Challenge Test (MCT)
A methacholine challenge test (MCT) is a type of lung function test. MCT is often done to diagnose asthma if symptoms aren't typical. If you have already been diagnosed with asthma, this test can be used to see if your medicine is working well and if your asthma is being controlled. It's also called a bronchoprovocation test.
How MCT is done
Your healthcare provider will have you breathe in (inhale) a small amount of methacholine. This is a medicine that causes the lungs’ airways to tighten (narrow), in the same way that asthma does. If you have asthma, your airways will narrow when you breathe in methacholine at a low concentration.
Before and after you breathe in the medicine, you will do a breathing test called spirometry. This measures how much air you can take into your lungs and how fast you can blow it out. This will show if your lung function changes at all. People with asthma have a decrease in lung function when even a small concentration of methacholine is inhaled.
Possible risks of MCT
This test is considered safe. But it can cause these reactions:
Your healthcare provider or a lab technician will watch you closely during the test. Let them know if you have any mild pain or breathing problems during the test. If test results show that methacholine caused a major drop in lung function or if you have respiratory symptoms, you will be given a medicine (bronchodilator). This will help open up your airways.
Do not have this test done if:
-
You are pregnant or think you could be
-
You are breastfeeding
-
You have blood pressure that is not controlled
-
You had a heart attack or stroke in the past 3 months
-
You have an aortic or brain aneurysm
-
Your lung function is very low after your first baseline spirometry test
There may be other reasons why you should not have this test. Talk with your healthcare provider about any concerns you may have.
Before the test
To get ready for the test:
-
Tell your healthcare provider about all the medicines you take. This includes prescription and over-the-counter medicines, vitamins, herbs, and other supplements. You may need to stop taking some or all of these before the test.
-
Tell your provider if you had a cold or an upper respiratory infection in the past 4 weeks.
-
Don’t eat or drink anything with caffeine for at least 4 hours before the test. This includes chocolate, coffee, tea, and soda.
-
Follow any other directions you are given for not eating or drinking before the test.
-
Don’t smoke for at least 6 hours before the test.
-
Don’t exercise for at least 6 hours before the test.
Follow any other directions you are given before the test.
During the test
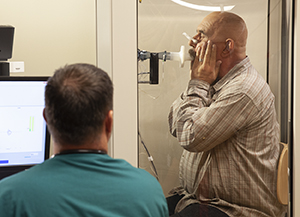
The test may be done in your healthcare provider’s office or in a pulmonary function lab. This is what you can expect:
-
You will first do a breathing test (spirometry). This will show how well your lungs are working and what your baseline lung function is. For this test, you will be asked to sit up straight. A clip is placed on your nose and you will be given a plastic mouthpiece connected to a spirometry machine. You will place your lips tightly around the mouthpiece to create a tight seal. You will take a deep breath and hold it for a few seconds. Then you will breathe out as hard as you can into the mouthpiece.
-
You will then breathe in a mist of methacholine through a nebulizer device.
-
If your lung function stays the same or you don’t have any symptoms, the healthcare provider will have you breathe in another low dose of methacholine.
-
You will be given the spirometry test again right after this.
-
If you don’t have a reaction to the methacholine, you will continue the test. After each breathing test, you will inhale a higher or stronger dose of the medicine. Then you will do a spirometry test.
-
Let the provider know if you have any mild pain or problems during the test. This includes feeling dizzy or lightheaded, having chest pain or tightness, coughing, wheezing, or shortness of breath.
-
The provider will stop the test if you start to have respiratory symptoms. These include wheezing, chest pain, coughing, or shortness of breath. Or they will stop the test when the spirometry shows major narrowing of the airways.
-
After the test is done, you will be given a medicine (bronchodilator) to reopen your lungs.
-
Another breathing test will be done to be sure your lungs are back to normal.
-
You will stay in the test area until your breathing is back to normal. You may be asked to wait for an hour or longer until you can go home.
After the test
After the test, you can go back to your normal diet and activity. You can take your medicines again unless your healthcare provider tells you otherwise.
Your provider will talk with you about your test results. The test is positive if the methacholine reduces your breathing ability by 20% or more, compared with your baseline. A positive test result means you may have asthma. A negative test result means you likely don’t have asthma.
Online Medical Reviewer:
Andrew D Schriber MD
Online Medical Reviewer:
Jessica Gotwals RN BSN MPH
Online Medical Reviewer:
Melinda Murray Ratini DO
Date Last Reviewed:
12/1/2022
© 2000-2024 The StayWell Company, LLC. All rights reserved. This information is not intended as a substitute for professional medical care. Always follow your healthcare professional's instructions.